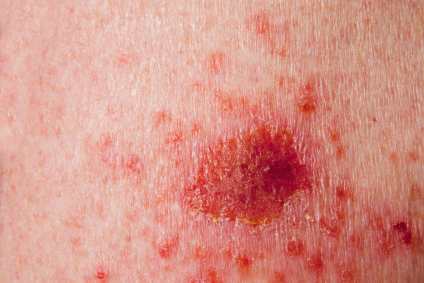
Accounting for greater than 90% of all skin cancers occurring among Americans, basal cell carcinoma (BCC) is the most prevalent type. While it rarely metastasizes (spreads) to other sites in the body, BCC may cause damage to surrounding tissues. Find out about the warning signs of BCC, the causes of BCC, risk factors for BCC, and BCC prevention measures.
Generalized Warning Signs of BCC
Basal cell carcinoma generally progresses slowly. In many cases, it causes no pain to the affected patient whatsoever. This particular type of skin cancer can look much the same as normal skin tissue, or it may be slightly raised or flat. However, bumps or growths may develop that have a distinct appearance. This includes:
- Light pink or white
- Waxy or pearly
- Brown or flesh colored
More Serious Warning Signs of BCC
- A sore on the skin that bleeds very easily
- A sore that persists and does not heal properly
- A sore which oozes or has crusty spots
- A sore resembling a scar when there is no injury to the area.
- Blood vessels with an irregular appearance either within or surrounding the sore
- A sore that has a depressed (sunken) center
The Causes of BCC
While the causes of many types of cancers are not known, the specific cause of BCC is harmful ultraviolet rays from the sun or the use of tanning beds. When these rays come in contact with the skin, they damage each skin cell’s DNA. The body attempts to fix the skin damage, but when it is repeatedly exposed, it can no longer adequately repair itself.
When the body can no longer repair the damage caused by ultraviolet rays, skin cancer develops. Generally speaking, BCC skin cancer tends to appear many years after the initial overexposure to the sun or tanning beds. When a patient reaches approximately fifty years of age, chances of developing BCC and other skin cancers are significantly increased. Younger individuals can also develop basal cell carcinoma. The majority of those affected are younger women who make use of indoor tanning beds. Most of these BCCs are preventable by never starting to tan indoors at all.
Risk Factors for BCC
All people can develop BCC, the most common form of skin cancer. However, some individuals are at an increased risk for developing basal cell carcinoma. Patients with risk factors for BCC have at least one or more contributing factors: their individual physical traits, taking part in activities which lead to BCC, and their personal medical history.
Personal Physical Traits
- Skin complexion – light skin and/or freckles
- Eye color – gray, blue or green
- Hair color – blonde or red colored hair
- Easily sunburned – having a tendency to sunburn rather than tan
Contributing Activities
Two main activities, both in the past and the present, can significantly contribute to any patient getting basal cell carcinoma. These include:
- Sun exposure – spending a considerable amount of time outdoors for either leisure or work purposes without using the appropriate measures (sunscreen and proper clothing including hats, long sleeved tops and pants)
- Tanning equipment exposure – frequent use of a tanning bed or sun lamp
Medical History
Several aspects of a person’s past medical history can make them more susceptible to basal cell carcinoma than other people. These include:
- Previous BCC – having a history of skin lesions increases your risk for developing subsequent instances by as much as 40%
- Heredity – having a close family member with BCC
- Immunosuppressant drugs – organ recipients and those with severe cases of arthritis, lymphoma or HIV often take medications that suppress their immune systems
- Excessive radiation exposure – having numerous X-rays or anyone who received X-rays to treat acne in the 1940s
Prevention of BCC
The best way to lower your chances of getting BCC if you are “at risk” is to avoid exposure to the sun as much as possible. Regular skin checks are also an excellent way to prevent BCC. A patient or their partner can check for signs of BCC at home, too. Dermatologists recommend that you go to your family doctor or dermatologist for frequent skin cancer checkups. Other preventative strategies include:
- Limiting sun exposure – avoid excessive sun especially for recreation
- Avoid peak sun times – peak time is between 12 noon and 2 PM
- Wear protective clothing – wide brimmed hats and protective skin coverings
- Use sunscreen – routine use of either waterproof or water resistant sunscreens containing UVA/UVB protection and a SPF factor of 30 or more
- Tell your doctor about lesions –suspicious appearing and/or changing lesions